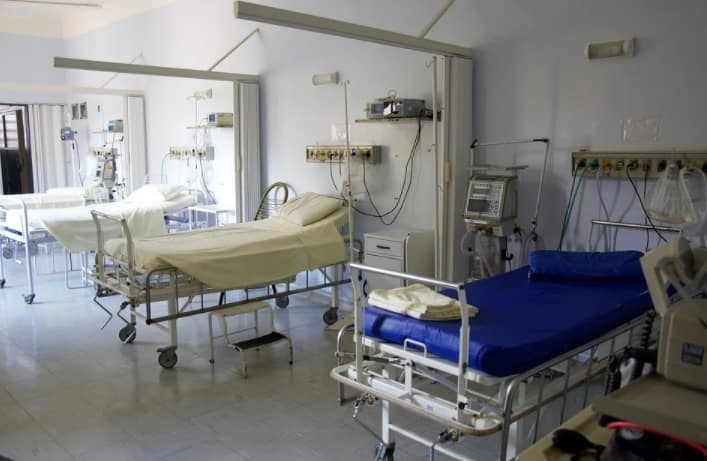
A Review of Healthcare Fraud in the United States
- in Health
Healthcare fraud in South Carolina and across the United States is a growing problem as the number of hospice patients has skyrocketed in recent decades. You can read more about this growing issue in an article on Hill Reporter. It’s also worth mentioning that the vast majority of people receiving hospital care benefit from the federal government through the Medicare or Medicaid programs. In this article, we will look at healthcare fraud in the United States in recent years.
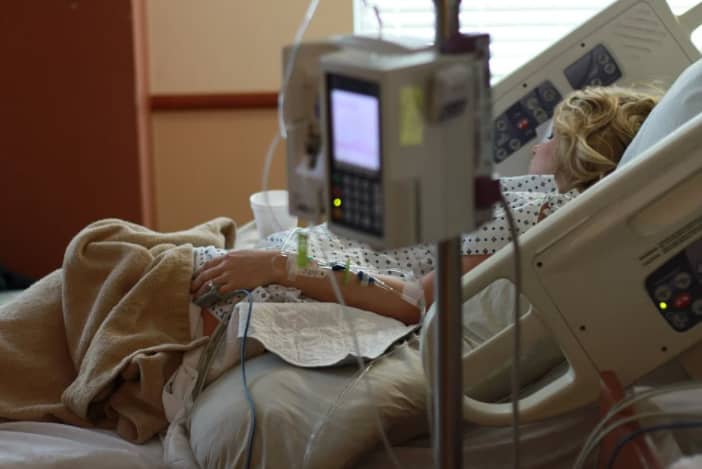
Introduction to Healthcare Fraud
Most hospice organizations provide ethical and appropriate treatment to their patients because hospice eligibility under Medicare and Medicaid involves clinical decisions that can result in obligations of significant sums of money from federal agencies. There are tremendous opportunities for fraudulent practices and false billing claims by unscrupulous hospice providers. As recent federal hospice fraud enforcement actions have shown, the number of healthcare companies and those who like to attempt to defraud the Medicare and Medicaid hospice benefits program is on the rise.
A recent case of hospice fraud among a South Carolina hospice is Southern Care, Inc., a hospice company that compensated $24.7 million to an FCA case in 2009. The alleged frauds were that patients were ineligible for hospice, for humor, were not terminally ill, the absence of signs of terminal illness, that the company marketed to potential patients with the guarantee of free medications, provided, and delivery of home care aides.
Consequences of Healthcare Fraud
 The U.S. and South Carolina customers, such as hospice patients and their families, and healthcare professionals involved in the hospice business should get used themselves to the basics of their hospice care companies, hospice eligibility under the Medicare and Medicaid programs, and hospice fraud schemes that have grown up across the country. Consumers must protect themselves from shady hospice providers.
The U.S. and South Carolina customers, such as hospice patients and their families, and healthcare professionals involved in the hospice business should get used themselves to the basics of their hospice care companies, hospice eligibility under the Medicare and Medicaid programs, and hospice fraud schemes that have grown up across the country. Consumers must protect themselves from shady hospice providers.
Furthermore, hospice workers must protect themselves from intentionally or knowingly engaging in health care fraud against federal regulators. They may expose themselves to administrative penalties, such as lengthy exemptions from working for a company that receives federal funds, huge fines and civil penalties, and criminal penalties, including imprisonment. Suppose a hospice employee identifies fraudulent conduct related to Medicare or Medicaid billings or claims. In that case, they should not engage in such conduct, and the criminal conduct must be reported to law enforcement and regulators.
Hospice Care Statistics
The number of times a patient receives palliative care is often referred to as “length of stay” or “length of care.” Length of stay depends on many specific factors, for example, but not limited to, the type and timing of illness, the caliber of accessibility to health care providers before palliative care referral, and the timing of palliative care referral. The median length of stay for palliative care patients was about 21 days. The normal length of stay was about 69 days, nearly 35% of palliative care patients were discharged within seven days after referral to palliative care.…